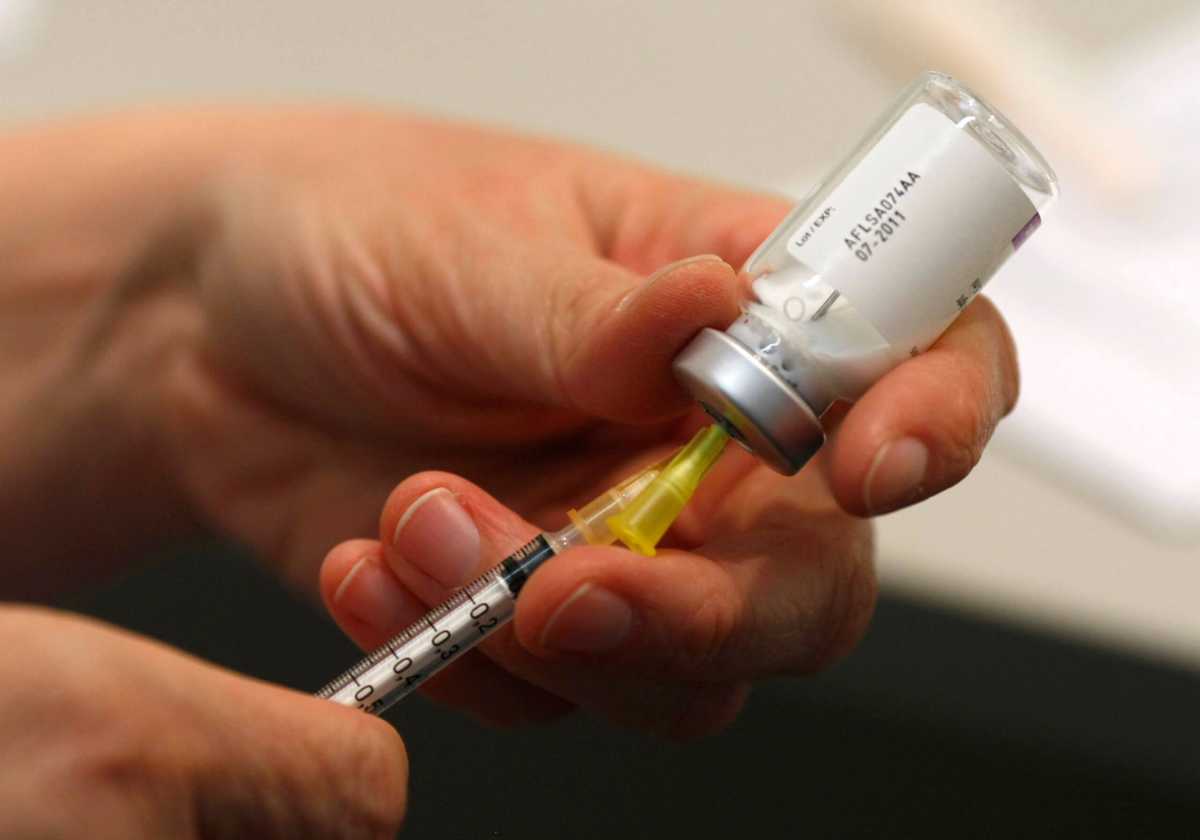
An HIV prevention shot administered once every other month is yielding more promising results among cisgender women in a clinical trial than PrEP pills, raising the possibility that the injection could eventually serve as an alternative to the rigorous daily regimen required for oral HIV prevention medication.
The trial, spearheaded by a global clinical network known as the HIV Prevention Trials Network (HPTN) and funded by the National Institutes of Health, the Bill and Melinda Gates Foundation, and ViiV Healthcare, compared the shot, which contains a drug called cabotegravir, with Truvada, the HIV prevention drug ingested orally.
Researchers ended their trial early after an independent monitoring board acknowledged encouraging results: The shot, manufactured by ViiV Healthcare, was found to be 89 percent more effective than Truvada. The news was first reported in The New York Times and additional information was provided in an announcement by HPTN on November 9.
Research indicates injection every other month is 89 percent more effective than Truvada
The trial was conducted across 20 locations and included women in Botswana, Eswatini, Kenya, Malawi, South Africa, Uganda, and Zimbabwe. Thirty-four women taking Truvada wound up testing positive for HIV, while just four women taking the shots contracted HIV, and two of those individuals had stopped receiving injections.
On average, participants were 26 years old, with more than half being 25 years or younger. Eighty-two percent were not living with a partner, 55 percent had at least two sexual partners in the previous month, and more than one-third had a primary partner who was living with HIV or did not know their status.
Notably, the shots would likely go a long way toward boosting adherence to HIV prevention medication.
“We know that adherence to a daily pill continues to be challenging, and an effective injectable product such as long-acting CAB is a very important additional HIV prevention option for them,” Dr. Sinéad Delany-Moretlwe, the trial’s protocol chair, said in a written statement. “We are grateful to the women who volunteered for this study and the research staff, as this study would not have been possible without their commitment to HIV prevention.”
The results represents a much-needed step forward in research surrounding HIV prevention medication among cisgender women, especially considering that girls and women represent about half of new HIV infections globally. As it stands, cisgender women are limited to taking Truvada, while men and transgender women have already been cleared to take Descovy as an alternative. Research surrounding HIV prevention medication for non-binary individuals and transgender men is also lacking.
HPTN also found success studying the shot’s effectiveness among cisgender men and transgender women who have sex with men in a separate study. A trial of nearly 4,600 individuals similarly found that the shot was 66 percent better than Truvada at preventing HIV among cisgender men and trans women.
The shot is one of multiple alternatives medical professionals have considered in response to the daily requirements of oral HIV prevention medication. Guidelines published by health officials in New York City and other areas have established a “PrEP on Demand” approach in which men who have sex with men can take two pills between two and 24 hours before having sex, one pill within 24 hours after sex, and another pill 24 hours after that. Should the individual have sex again the next day, he should continue taking PrEP daily until two days after sexual activity ends.
When that approach was unveiled, health officials limited their recommendation to cisgender men who have sex with men because they had yet to thoroughly examine PrEP on Demand’s impact on transgender individuals or cisgender women.
To sign up for the Gay City News email newsletter, visit gaycitynews.com/newsletter.